PhilHealth eClaims 3.0 is an Electronic Claims Submission System designed to automate the PhilHealth Members’ processing of eligibility and computations of the portion of Patient’s Billing which will be charged against PhilHealth. The system improves the operational efficiency and accuracy in the processing of Patient’s claims.
It contains Hospital Account module that monitors hospital’s account receivables and payments received from PhilHealth.
PhilHealth Accredited to eClaims 3.0 with Certificate No. 08-10-2018-00001
Alert Notification for Missing Data
PhilHealth eClaims 3.0 provides an Alert Notification to help reduce rejected claims due to incomplete, missing and invalid information. This feature helps minimize disruptions of hospital’s cash flow and increase the chance of getting paid by PhilHealth immediately. Claims submitted electronically are processed more quickly and accurately, resulting in faster payment.
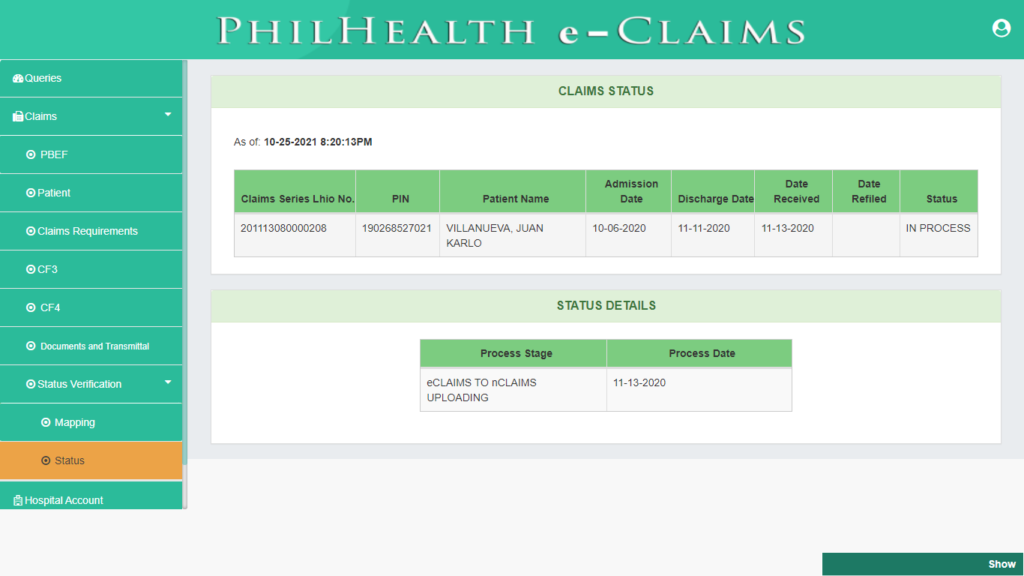
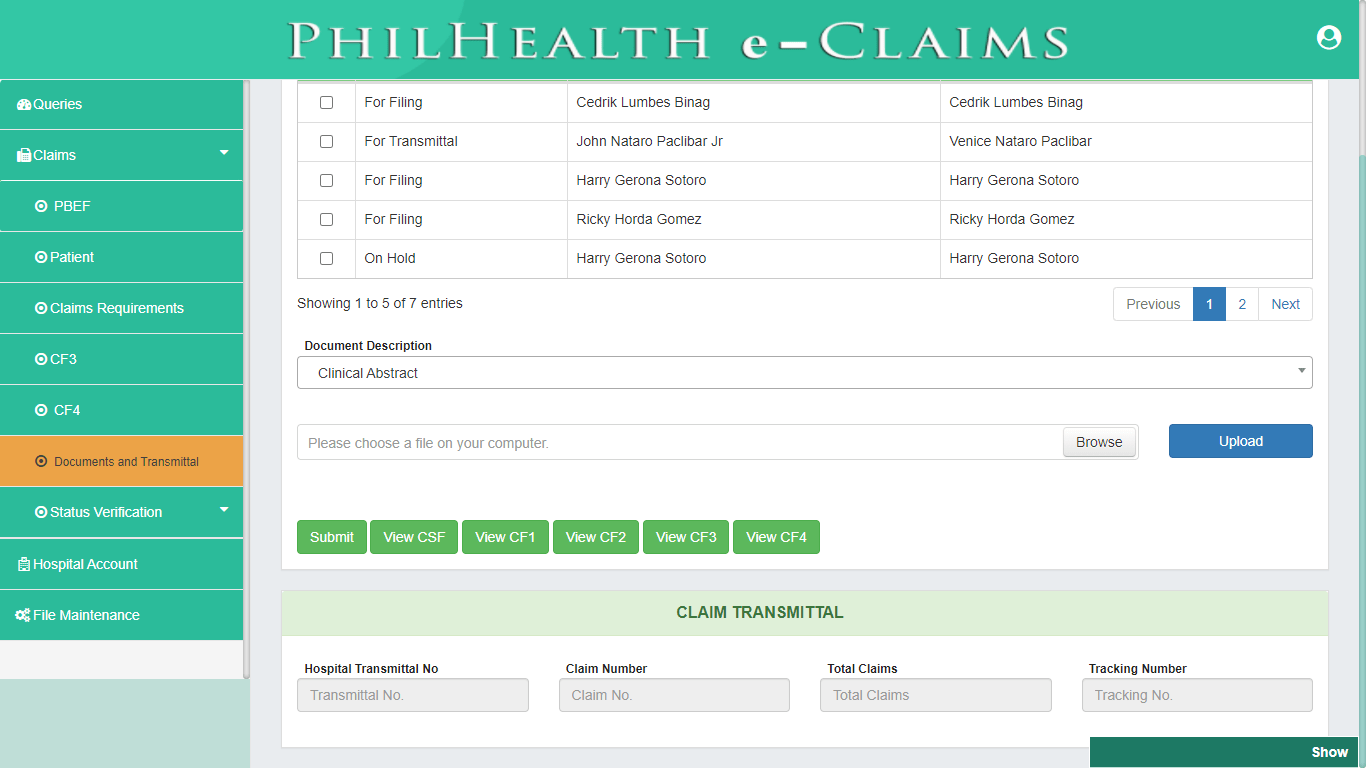
Real-Time Tracking of Claims Status
PhilHealth eClaims 3.0 provides real-time tracking of Claim Status. All claims filed to PhilHealth can be tracked using Status Verification module. Once the Claim Requirements has been submitted to PhilHealth using eClaims 3.0 it automatically generates a Receipt Ticket No. and Transmission Control No. that can be used for Tracking of Claim Status. Details of the claim status can be viewed such as Claims Series Lhio No. which is auto-generated by PhilHealth, Date of Submission of Claim, Process Stage, Process Date and Status of each Claim.
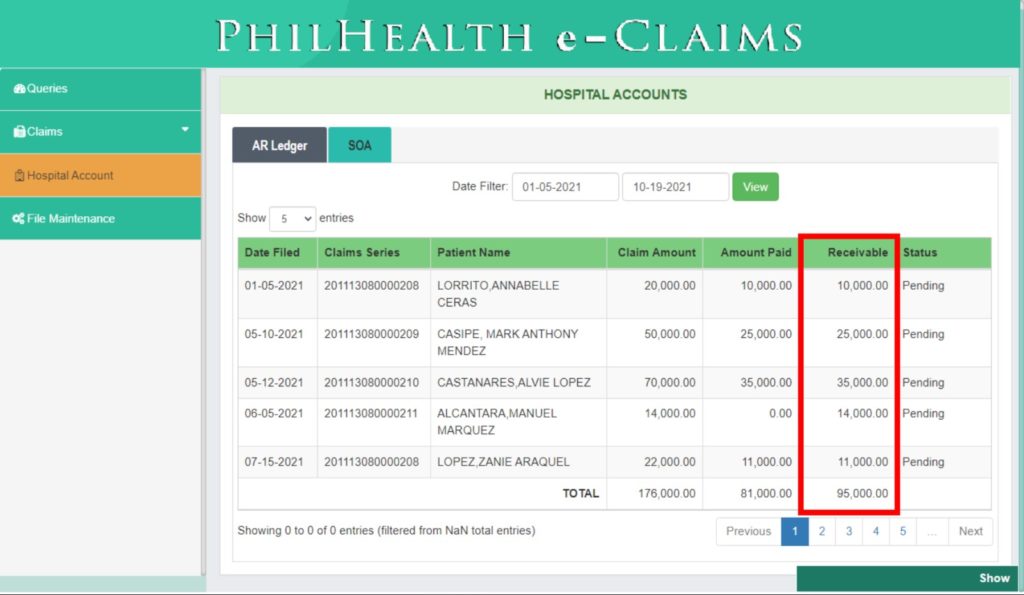
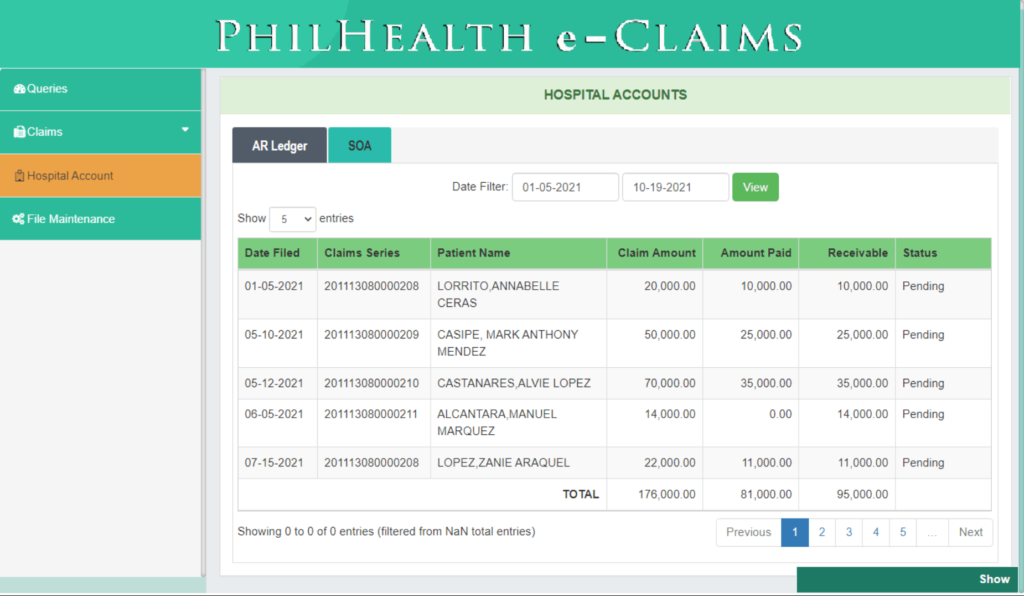
Monitoring of Hospital’s Account Receivables and Payments made by PhilHealth
PhilHealth eClaims 3.0 helps the Hospital to monitor their Account Receivables and Payments made by PhilHealth. It is able to generate a Statement of Account for Claim Reconciliation between the Health Care Institution and PhilHealth.
Paper Less Transaction
PhilHealth eClaims 3.0 eliminates the need to fill out and store paper claims, helping to streamline Claim processing and simplify record keeping.
Multi-level Security for Data Access
Components of PhilHealth eClaims 3.0
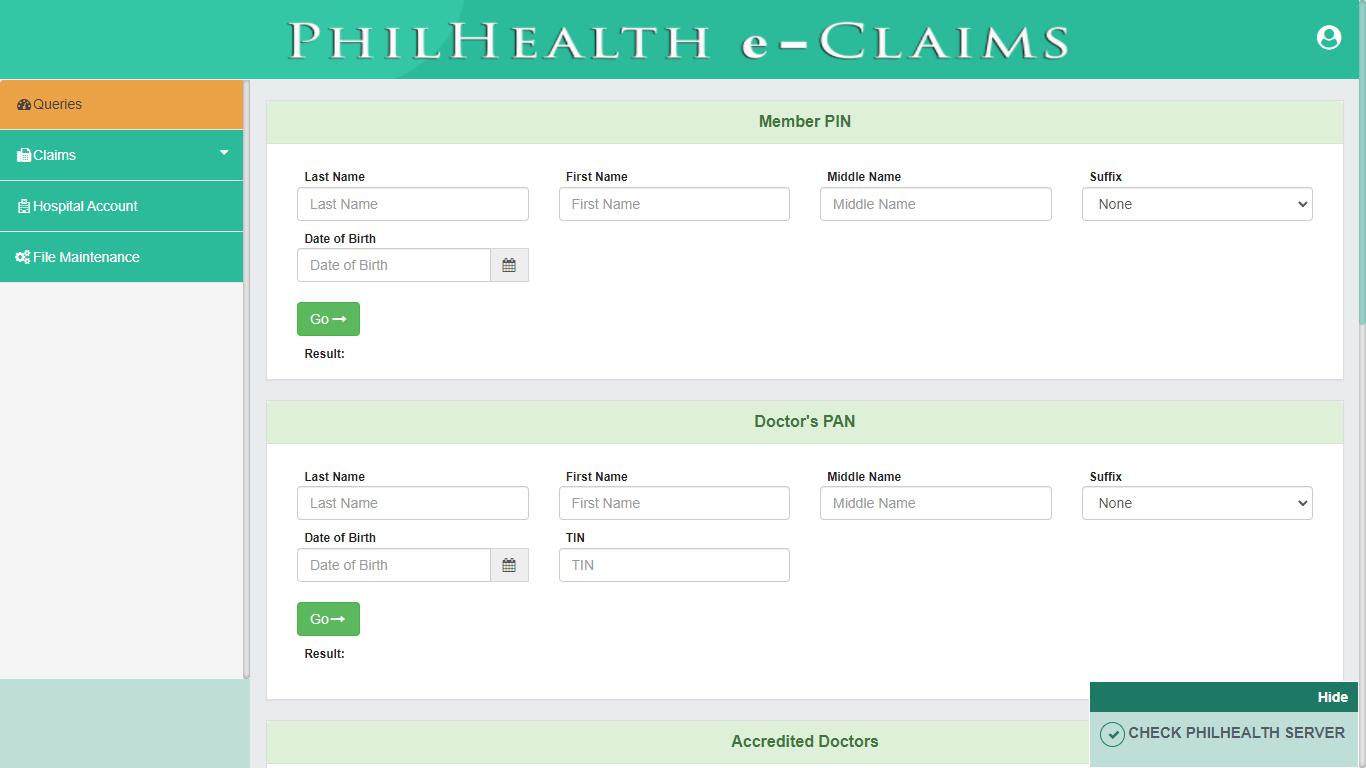
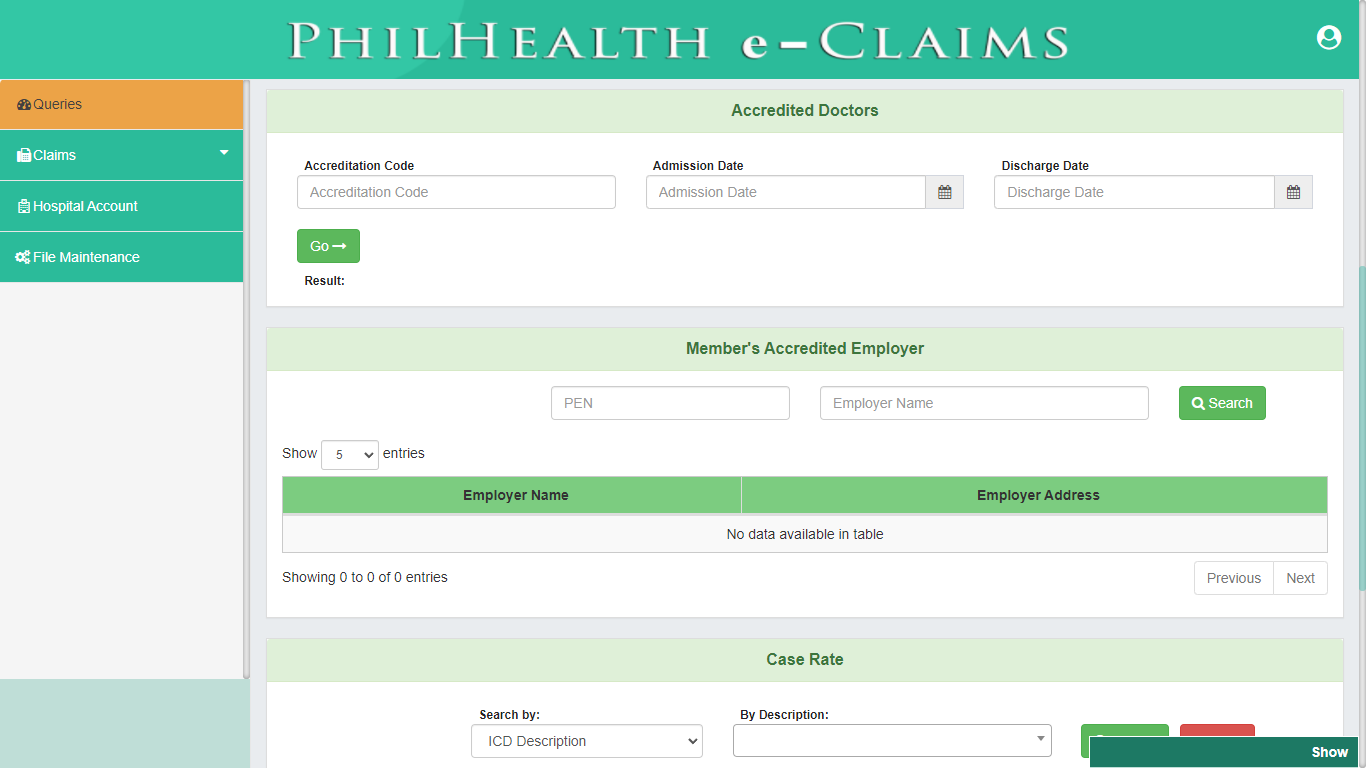
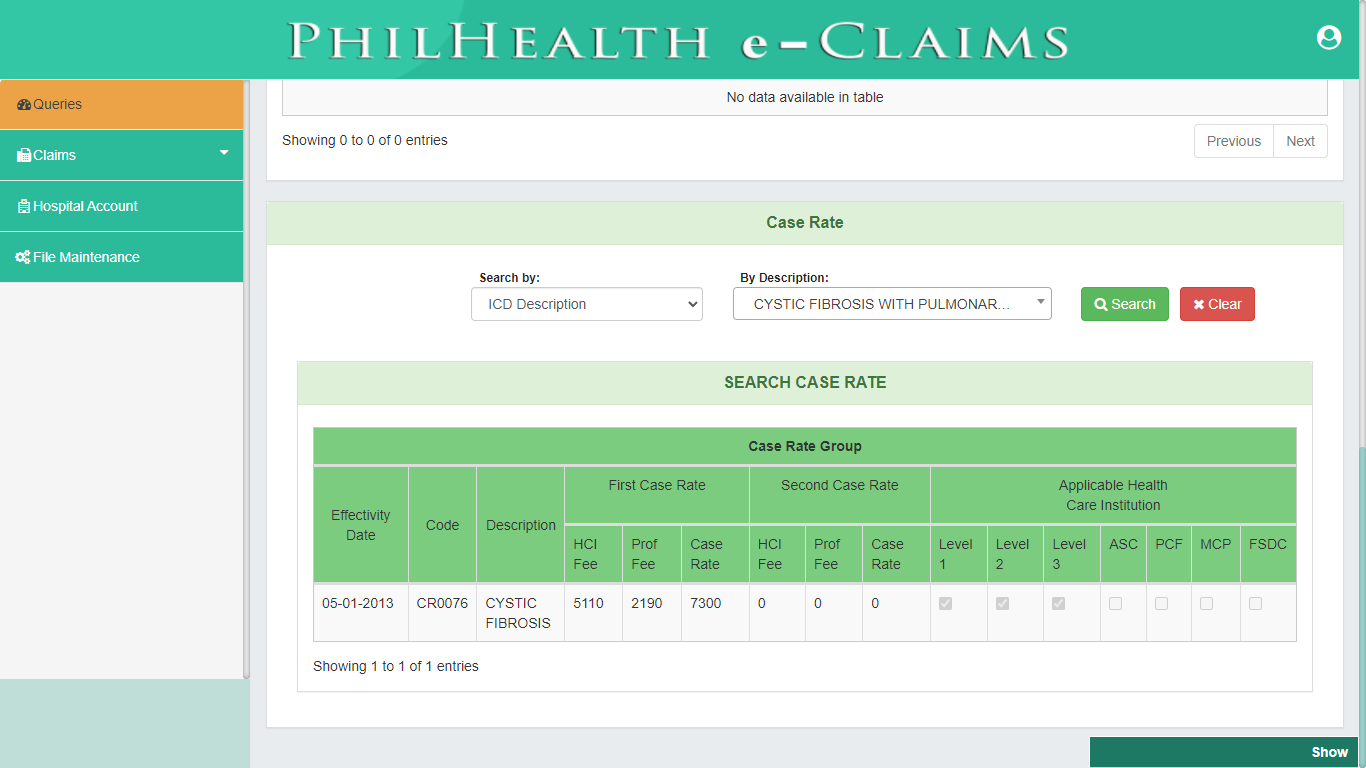
Queries
The main function of this module is to verify Member’s PhilHealth Identification Number (PIN), PhilHealth Employer Number (PEN) and Doctor’s PhilHealth Accreditation Number (PAN). This is composed of PIN Verification Utility, getting the Doctor’s PAN, Doctors Accreditation Check, Employer Accreditation Check and search for Case Rate.
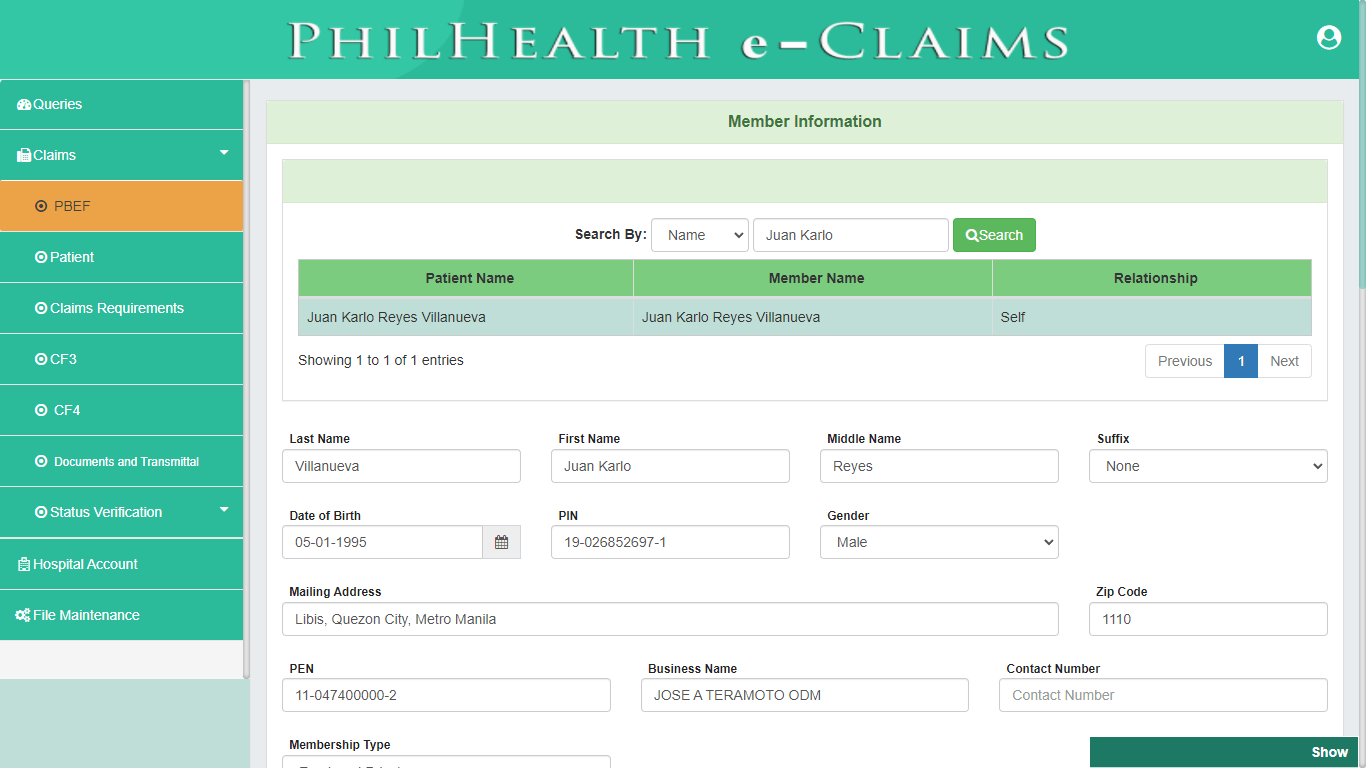
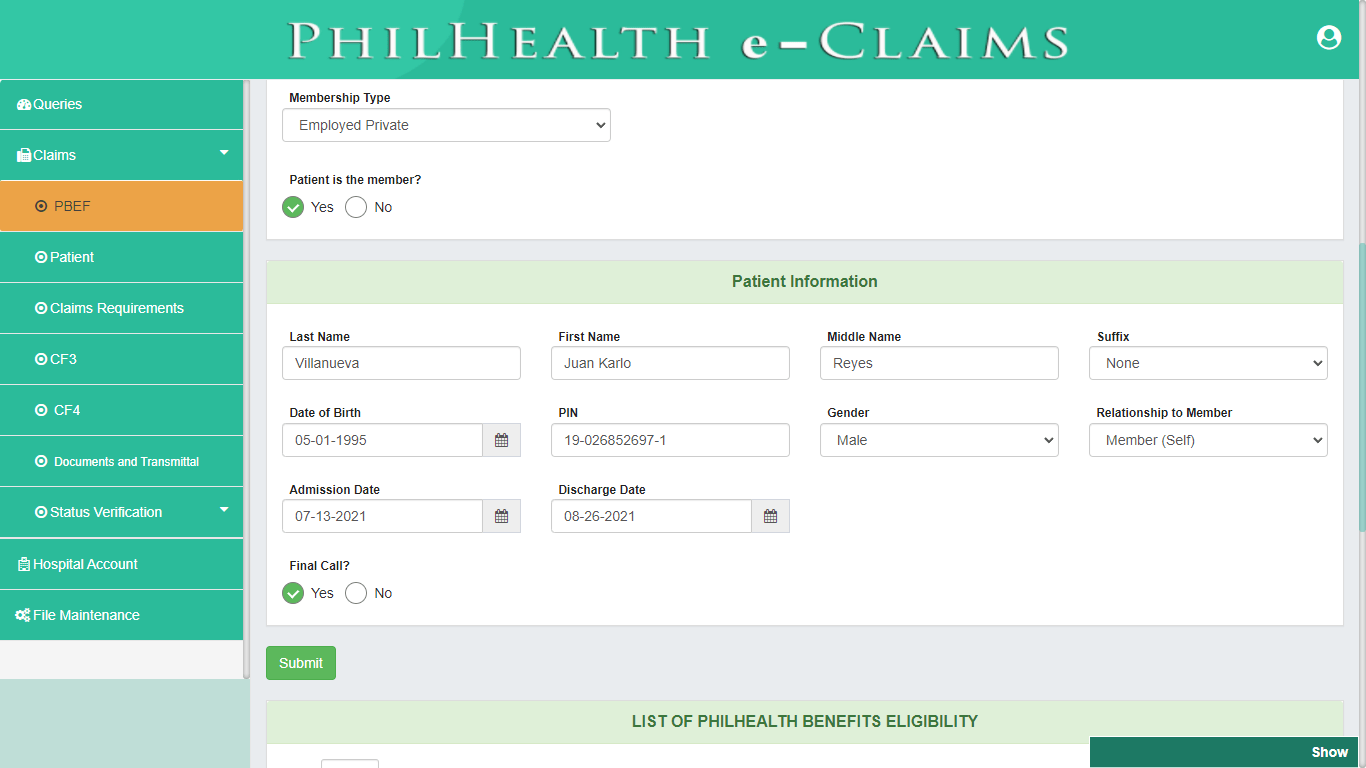
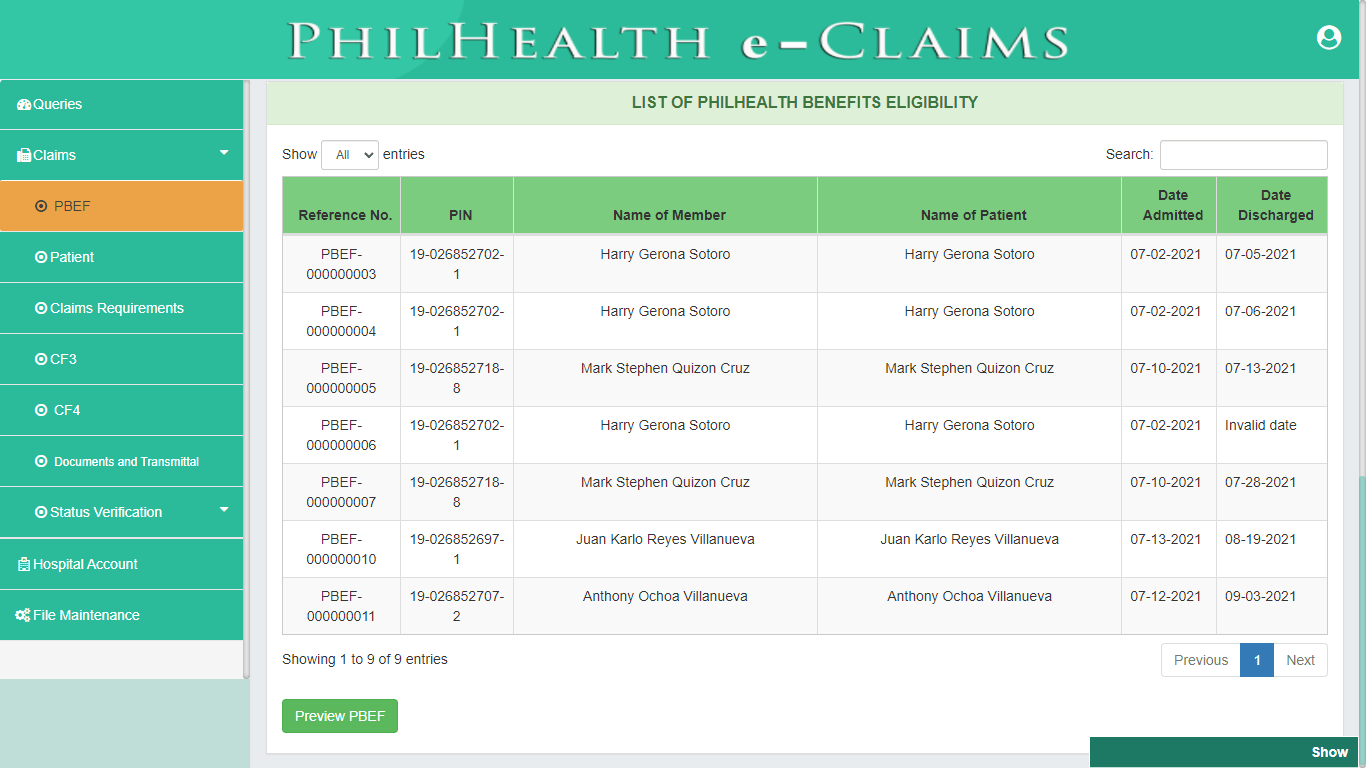
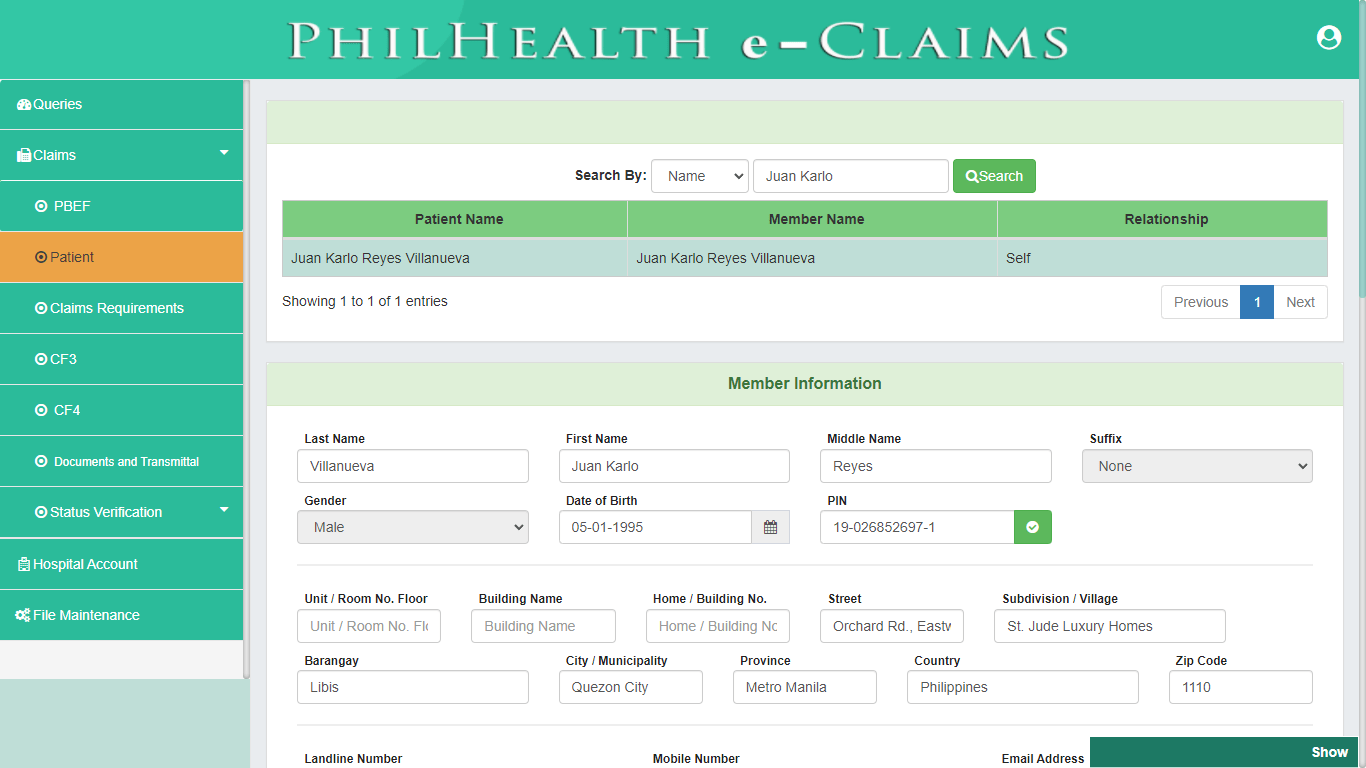
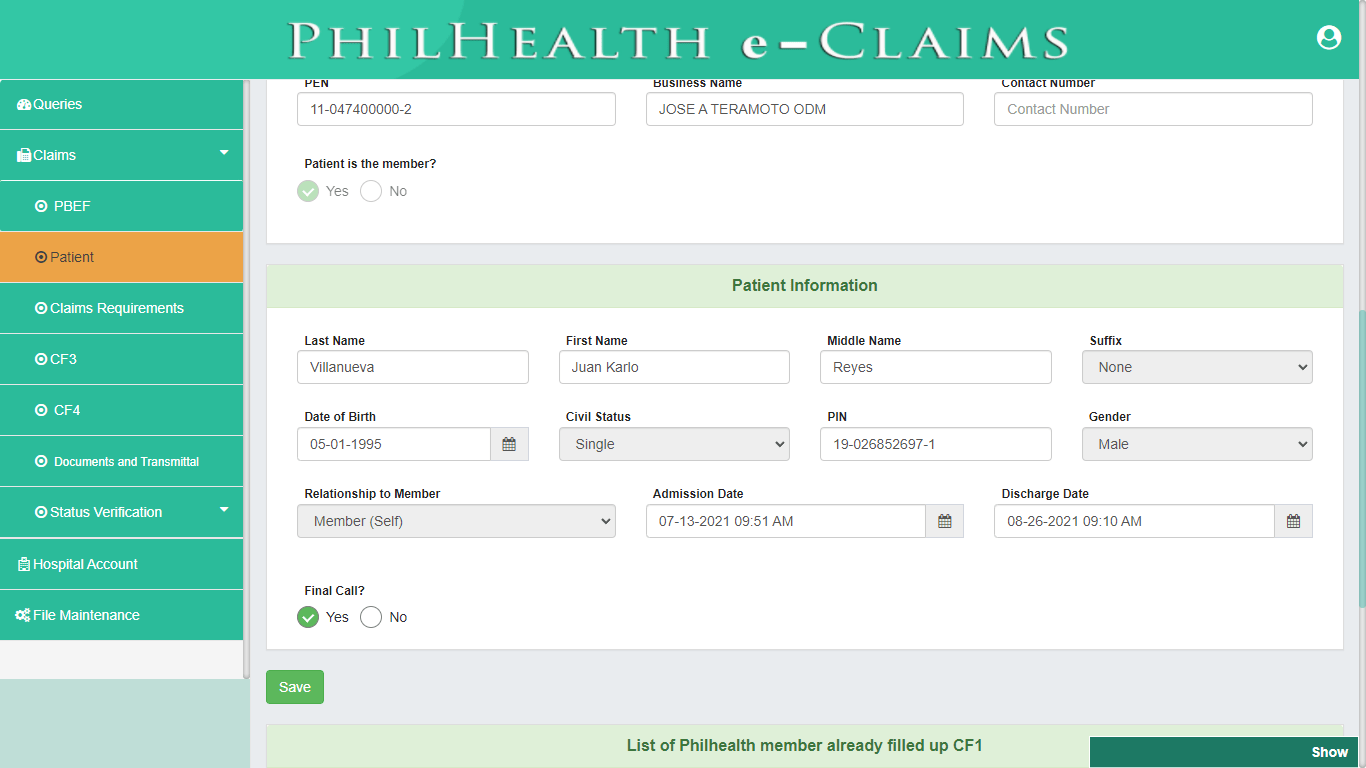
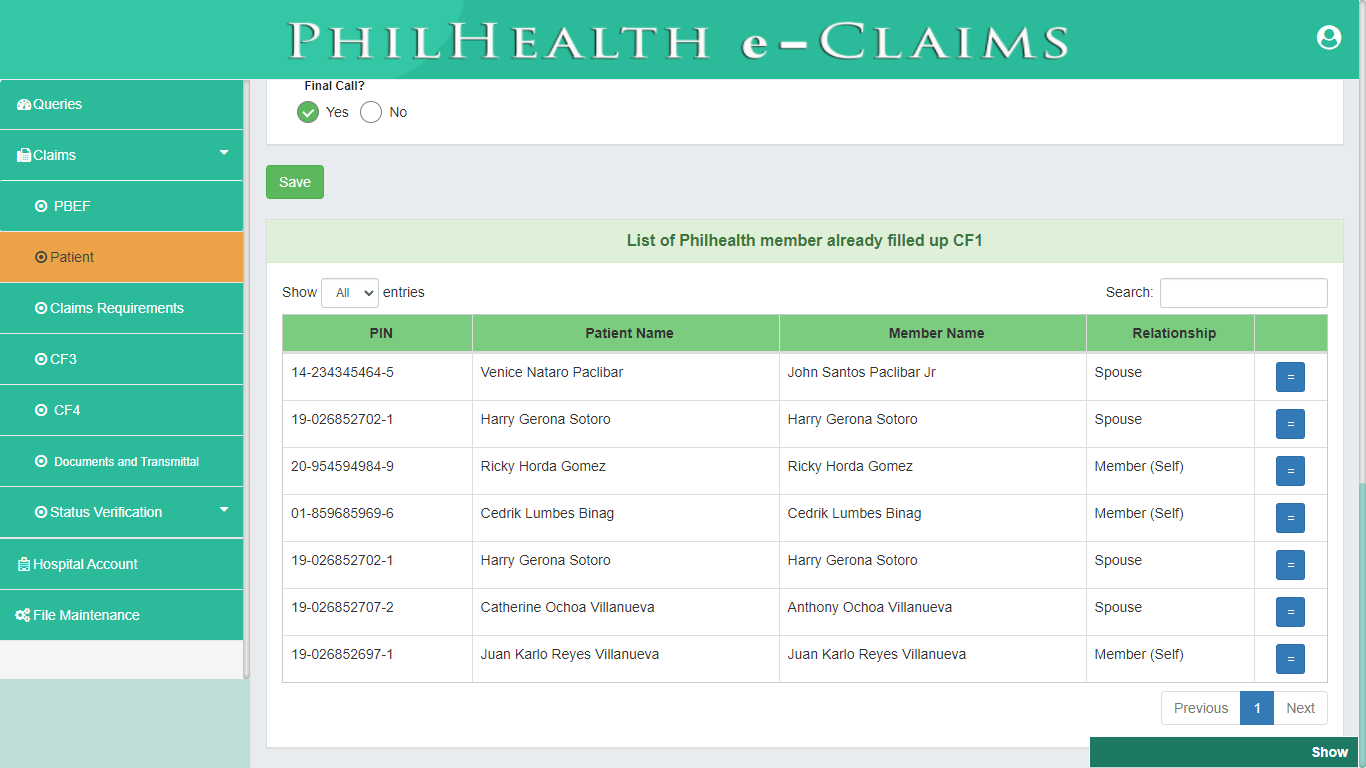
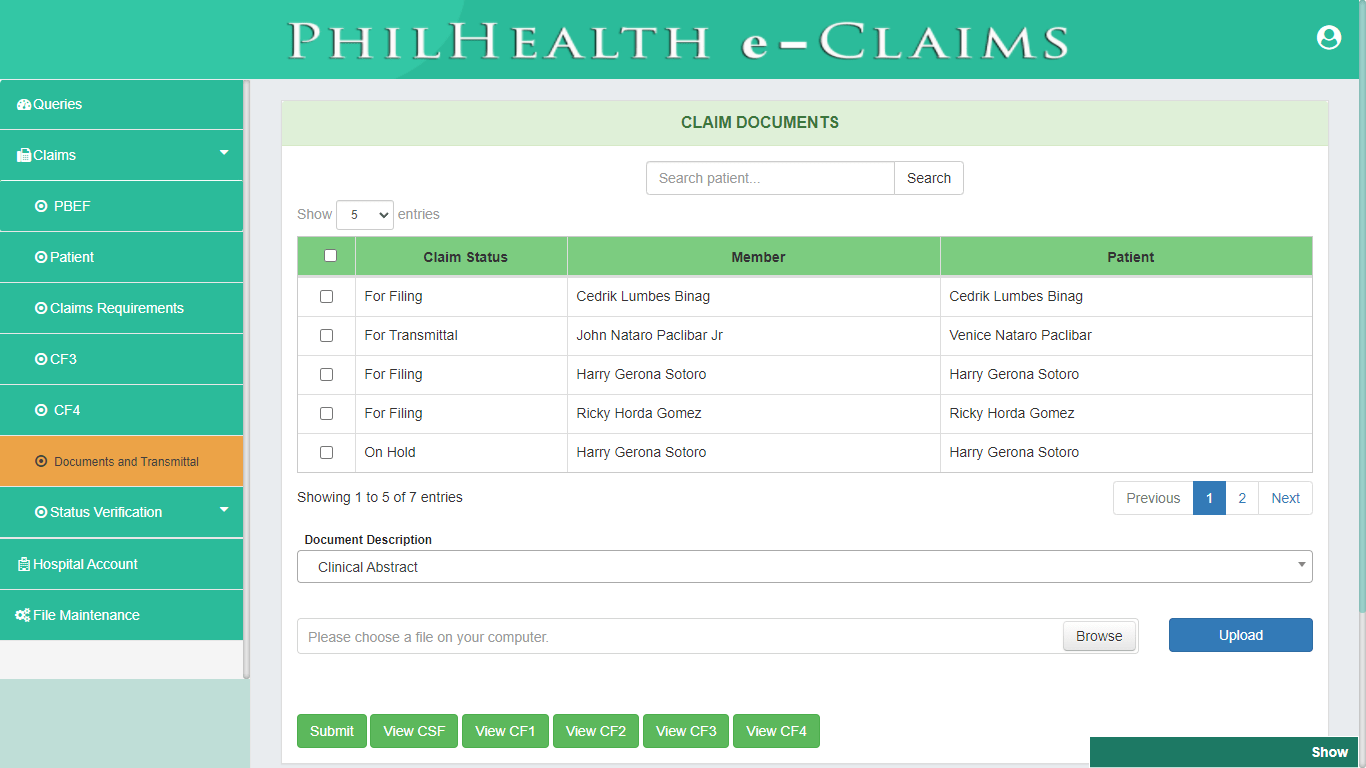
Patient (CSF, CF1)
Pursuant to PhilHealth Circular 2016-0016 on the full implementation of the Electronic Claims, Claim Signature Form (CSF) is one of the mandatory requirements in Claims adjudication. Patient module covers both the Claim Signature Form and Claim Form 1. Patient module validates status and profile information of Member Validity, Patient who is a dependent of a member, 45 days of confinement and Qualifying posted contribution. Claim Form 1 (CF1) is divided into two parts, Part 1 requires information about the Member and Patient to ascertain the identity of the Member, Patient, or Dependent for eligibility to PhilHealth benefits. The Second Part of CF1 provides the basic information about the employer and contains the certification of qualifying contributions.
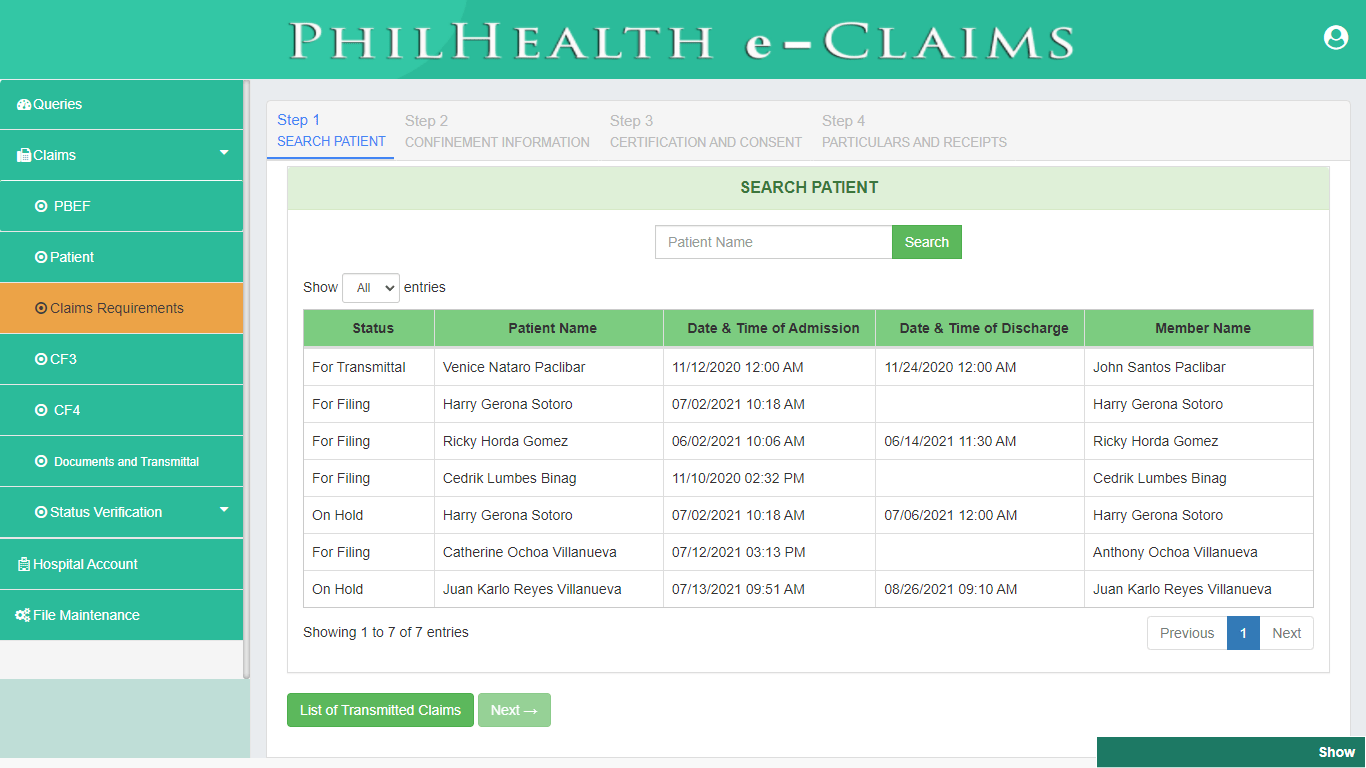
Claims Requirements (CF2)
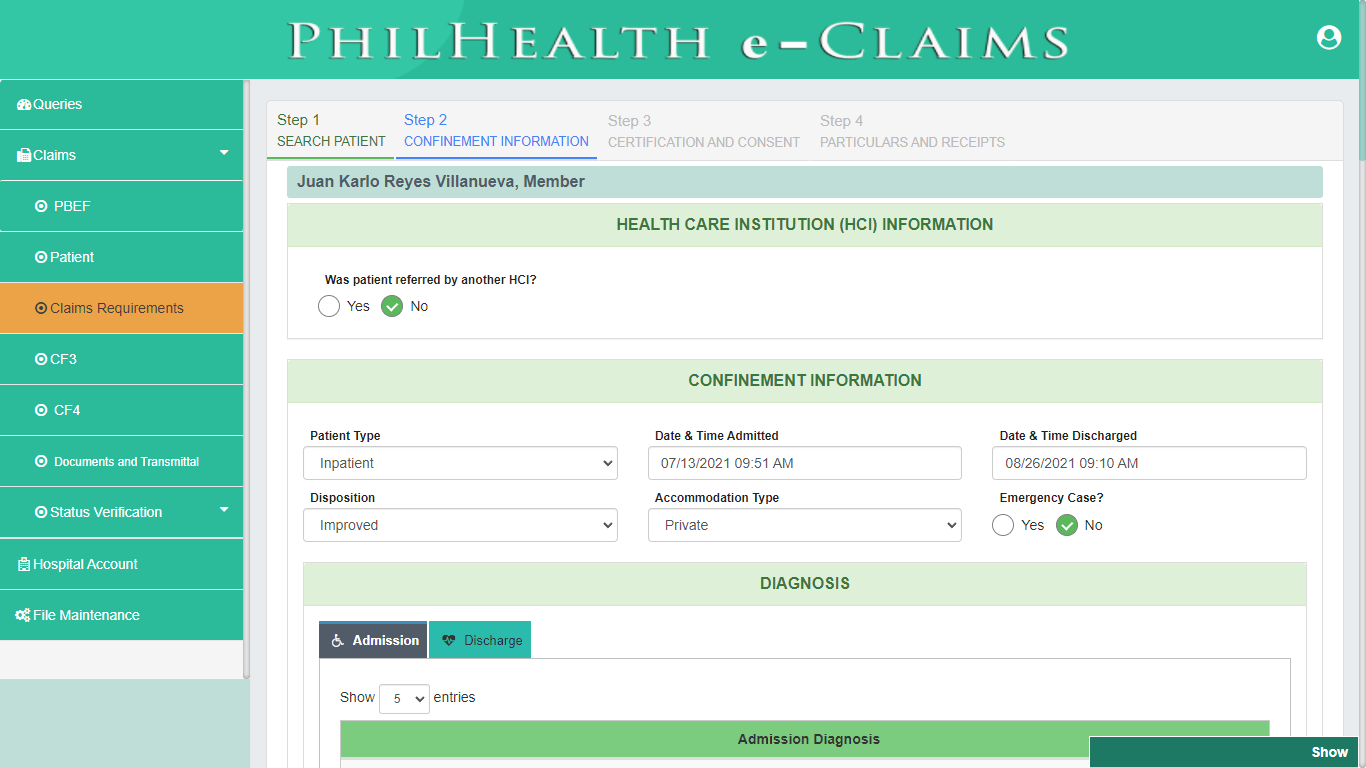
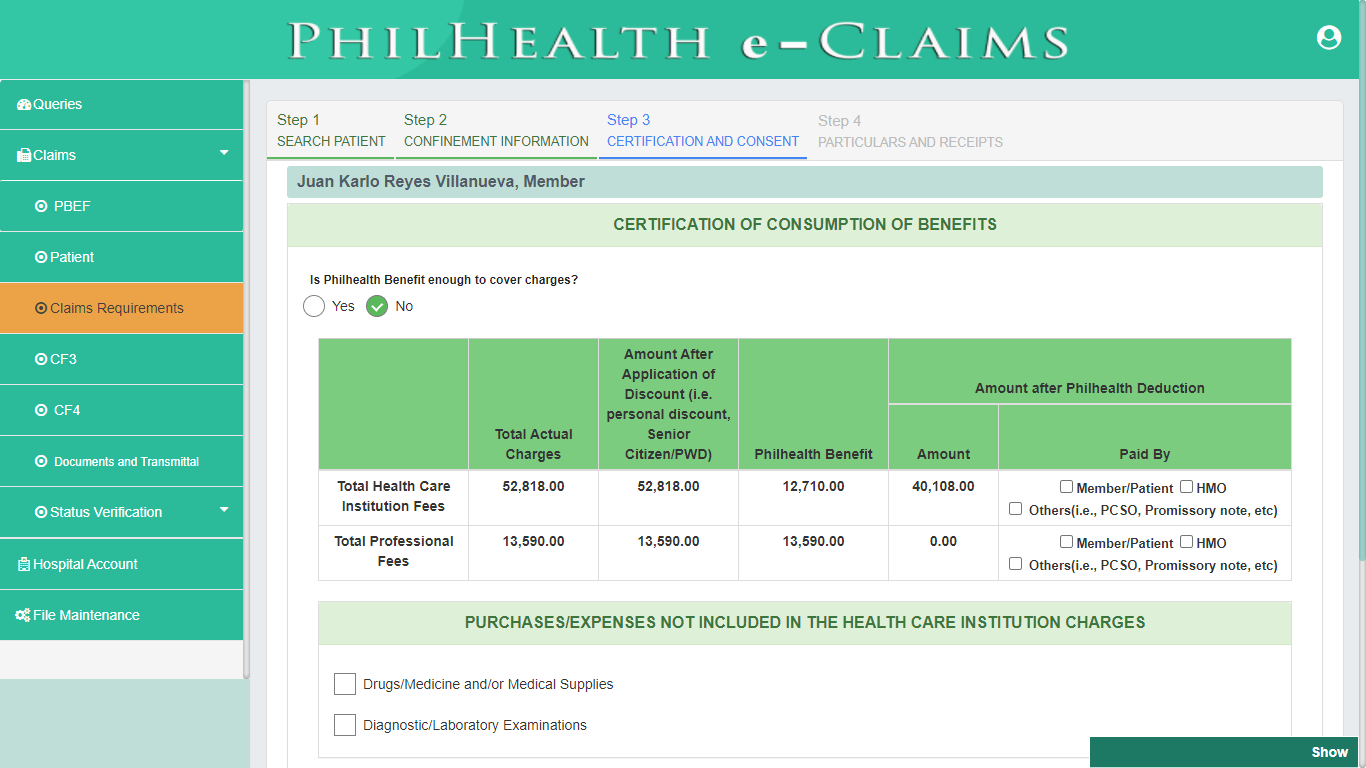
PhilHealth eClaims 3.0 provides a digital form of Claim Form 2. CF2 is a required document for PhilHealth Benefit Claims and is divided into 4 parts. Part 1 is the Health Care Institution Information which is not required to be filled out because the system automatically displays the information of the Health Care Institution. Part 2 is the Patient Confinement Information, Part 3 is the Certification of Consumption of Benefits and Consent to Access Patient Records and the last part of the form is the Certification of Consumption of Health Care Institution.
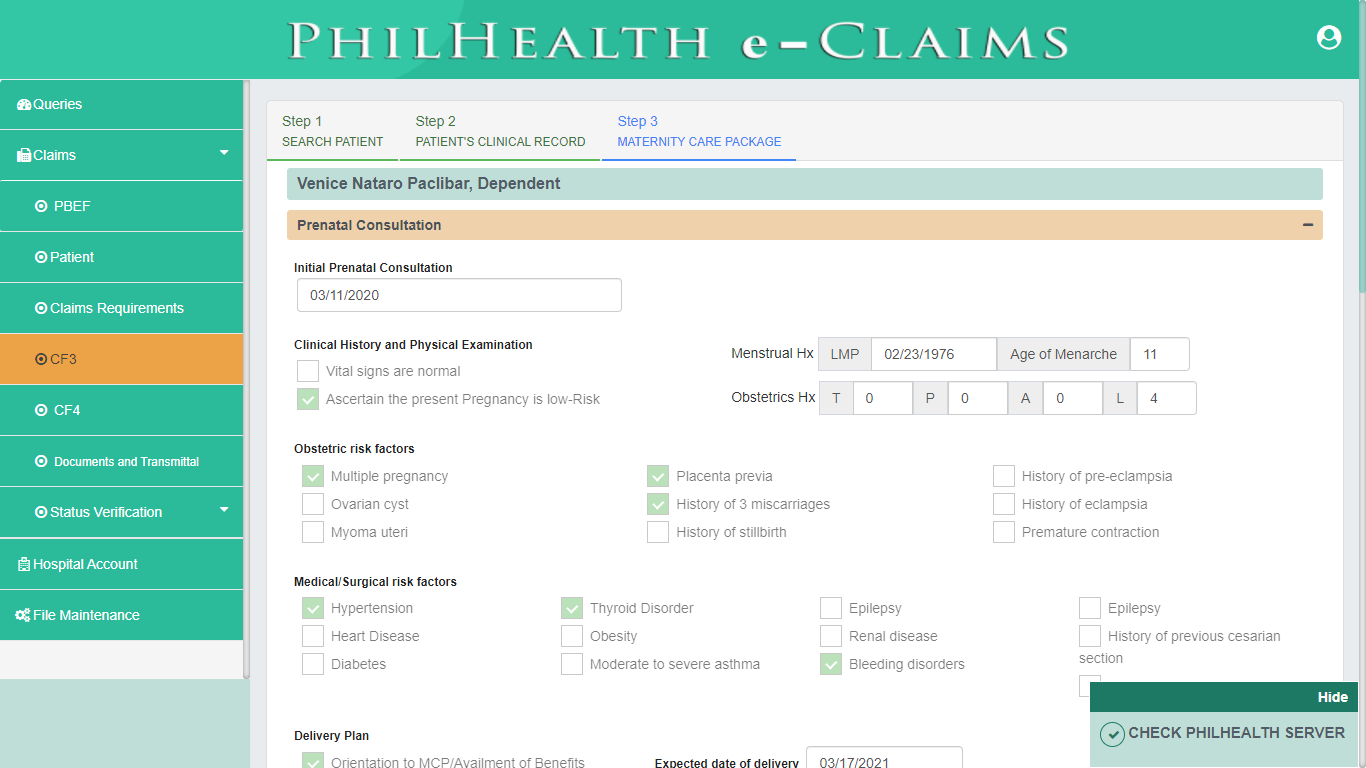
Maternity Care Package (CF3)
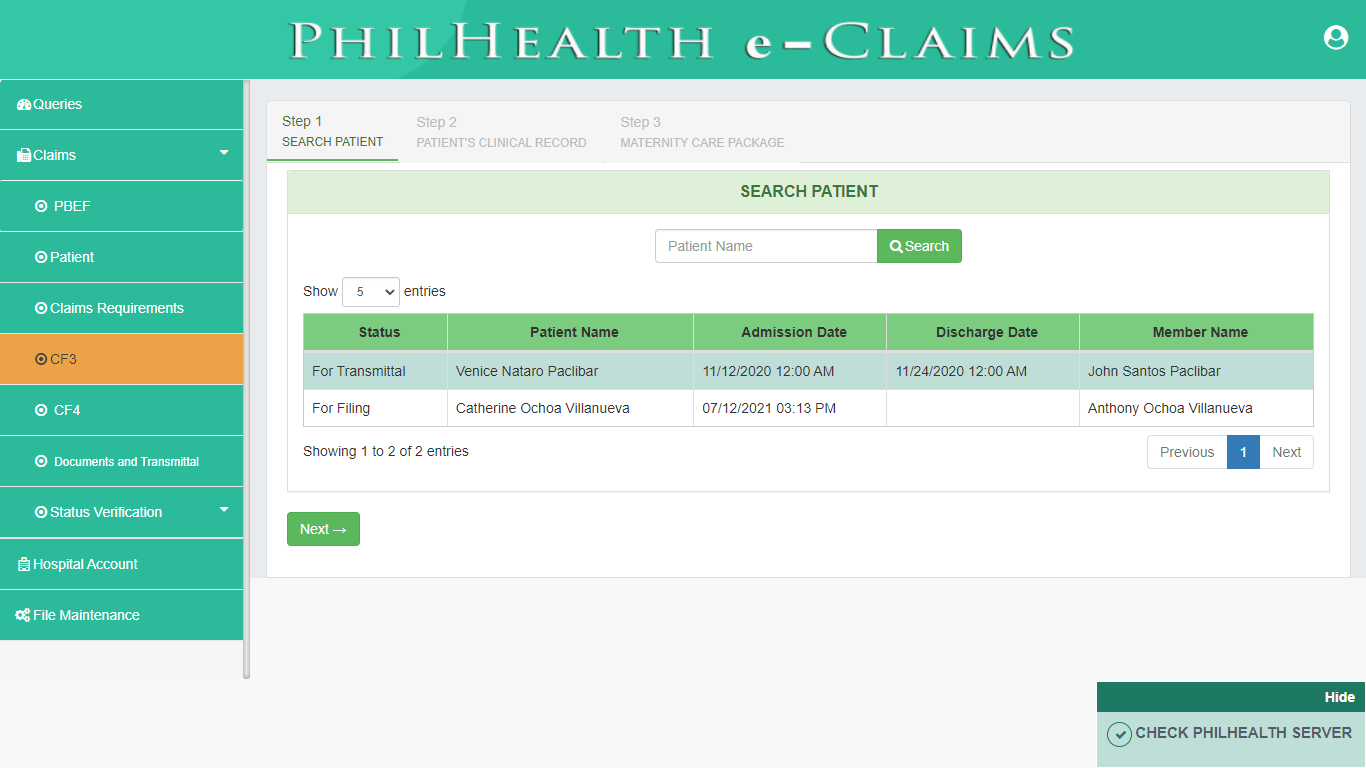
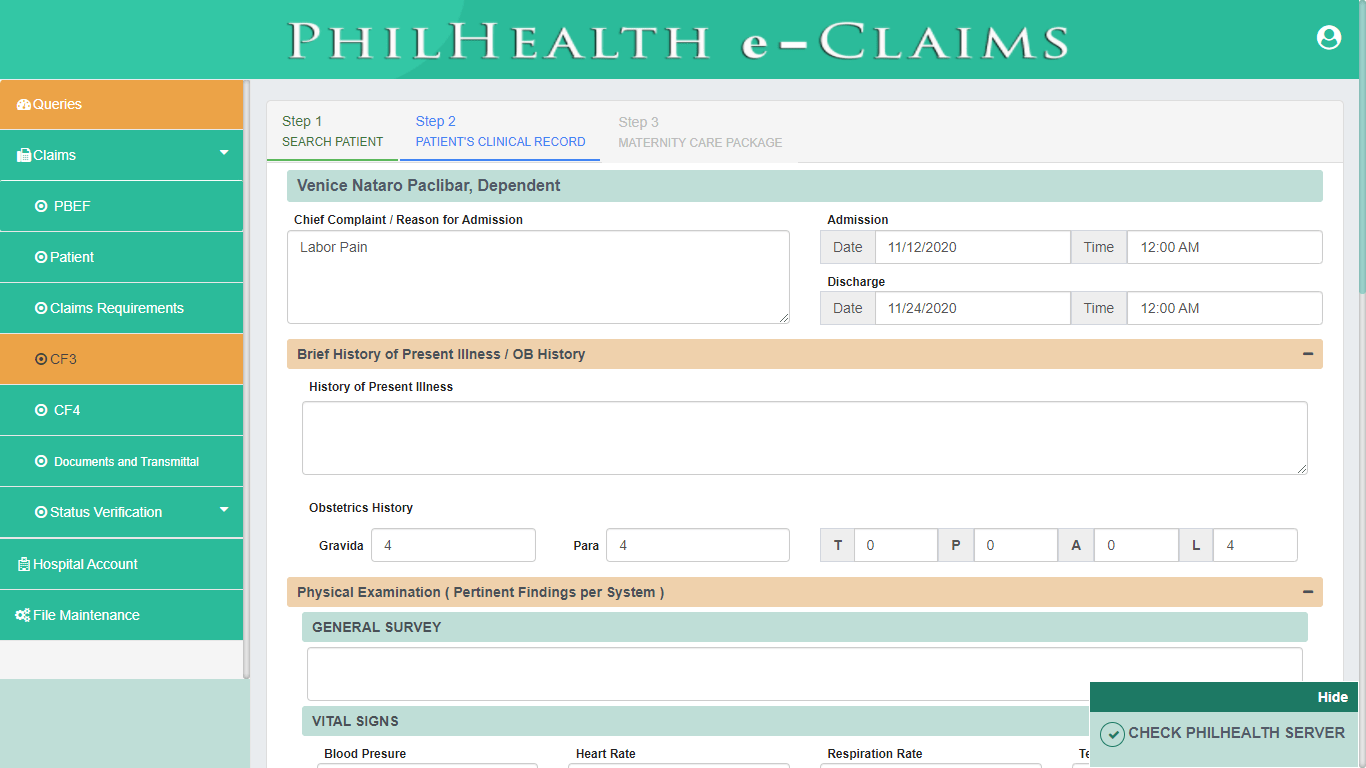
PhilHealth eClaims 3.0 provides a digital format of Claim Form 3. CF3 is only required for Maternity Care Package. Claim Form 3 is divided into 2 parts. First part of the form contains Clinical Record of the Patient while the Second part contains Maternity Care Package information such as Prenatal Consultation, Delivery Outcome and Postpartum Care.
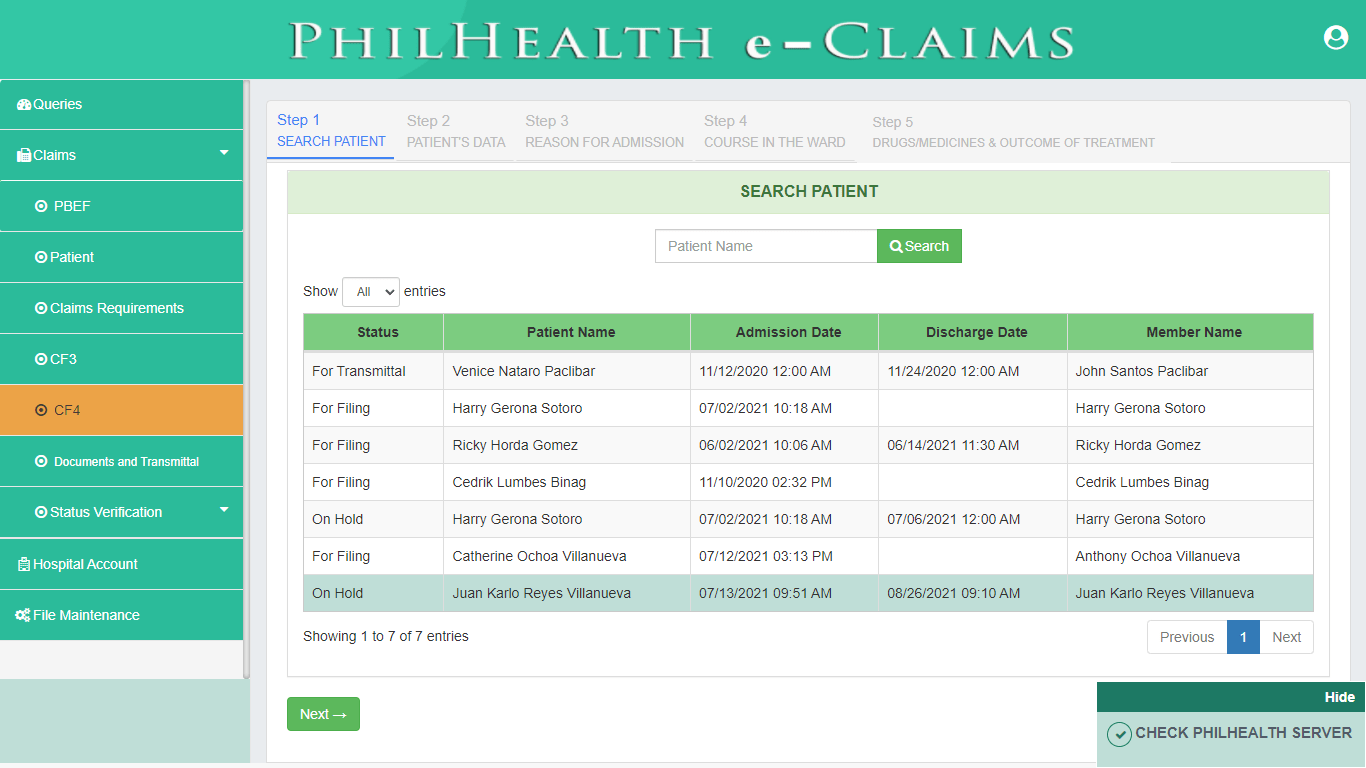
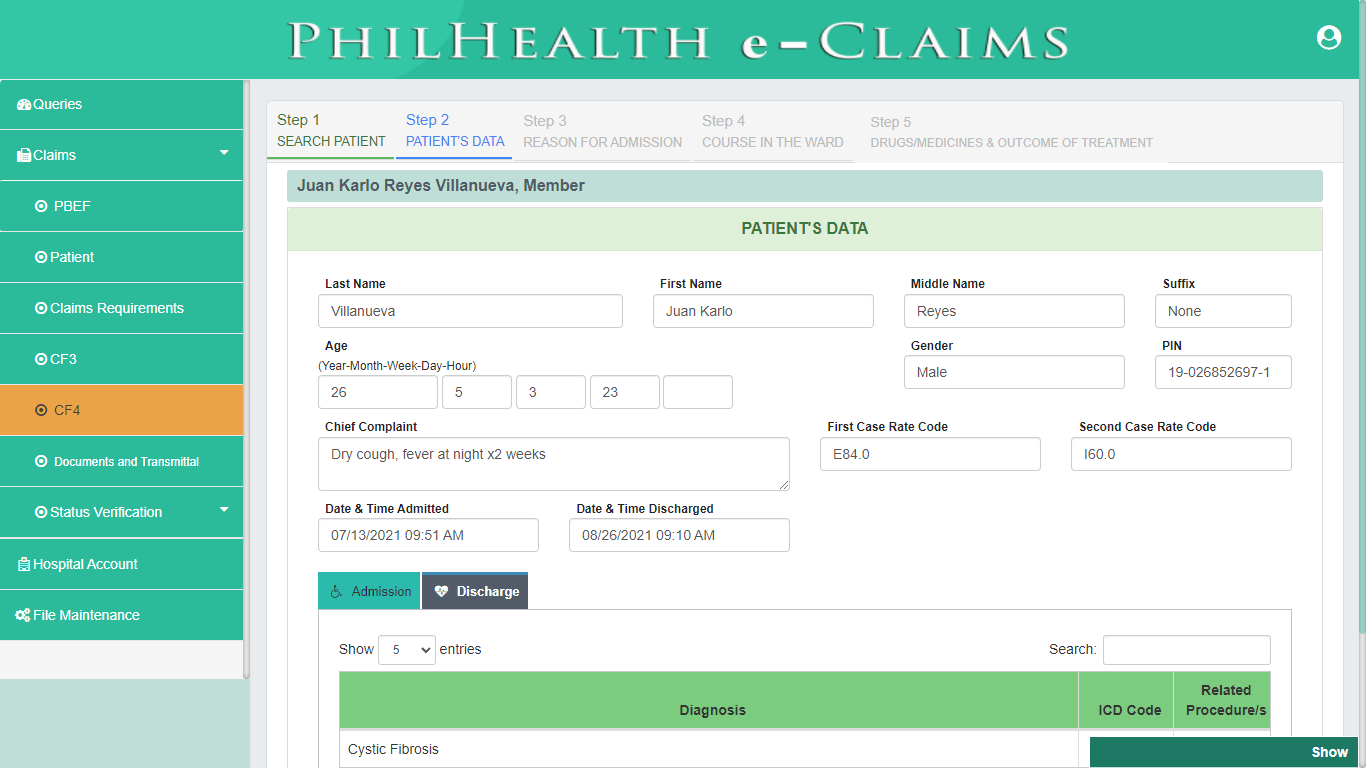
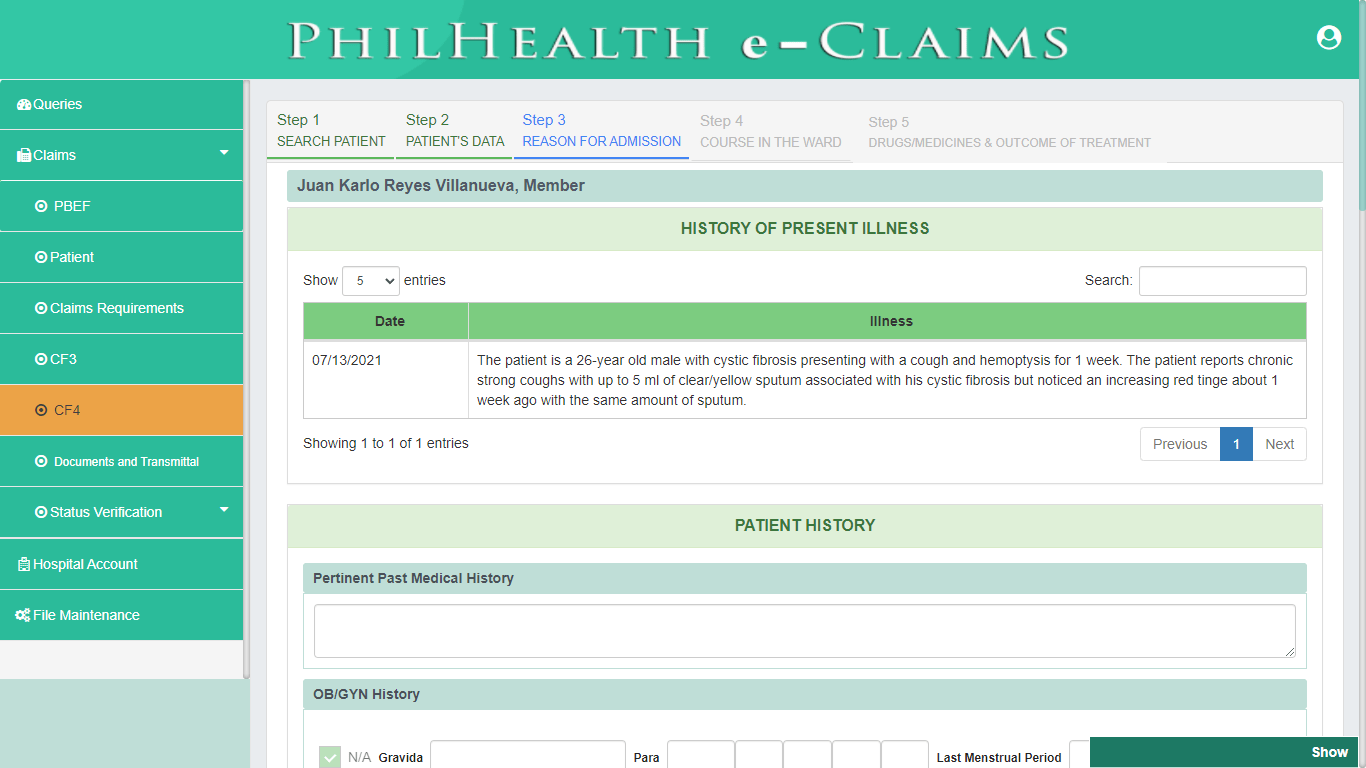
Claim Form (CF4)
PhilHealth eClaims 3.0 provides a digital format of Claim Form 4. CF4 is one of the requirements for PhilHealth Case Rate Claims. CF4 is the summary of Pertinent Clinical Information of Patient or Member during their hospitalization or episode of care that shall be utilized by PhilHealth to conduct evaluation and review of Claims.
Status Verification
PhilHealth eClaims 3.0 has Verification Status module designed for real-time checking of Claim Status. It contains a Mapping module that provides a List of Transmitted Claims with Receipt Ticket No., Transmission Control No., Transmission Date, Patient and Member’s Name. It also has Status module that provides Real-Time Checking of Claim Status.
Hospital Account
PhilHealth eClaims 3.0 provides a Hospital Account module designed to help the Hospital in monitoring their Account Receivables and Payments made by PhilHealth. Hospital Account module automatically generates a Statement of Account used for Claim Reconciliation between the Health Care Institution and PhilHealth.
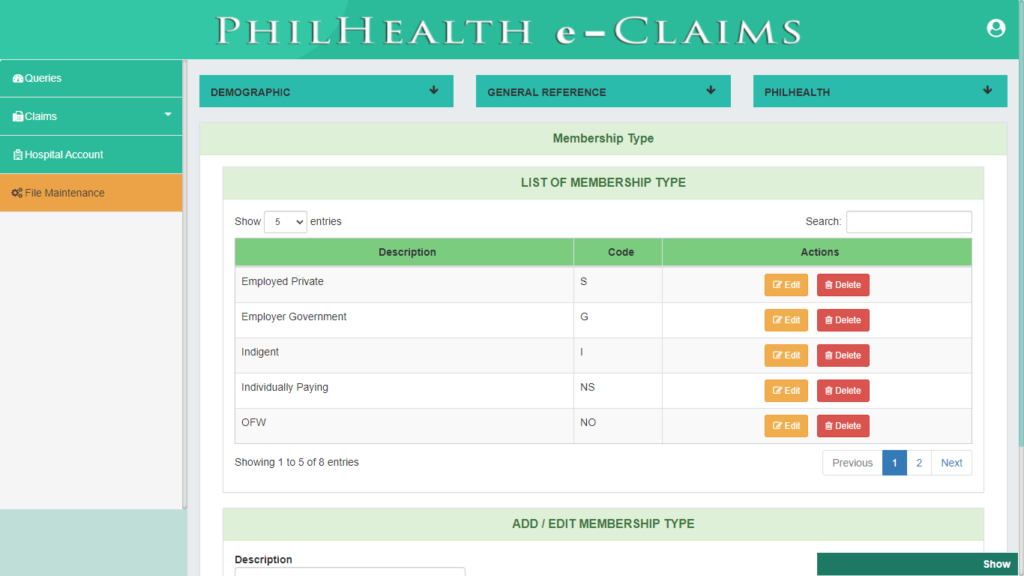
File Maintenance
File Maintenance contains all the pre-loaded Data Tables that are repeatable and displayed in Dropdowns & Checkboxes for fast encoding of records. Values from File Maintenance can also be viewed and displayed in Reports for dynamic, fast & easy report generation.
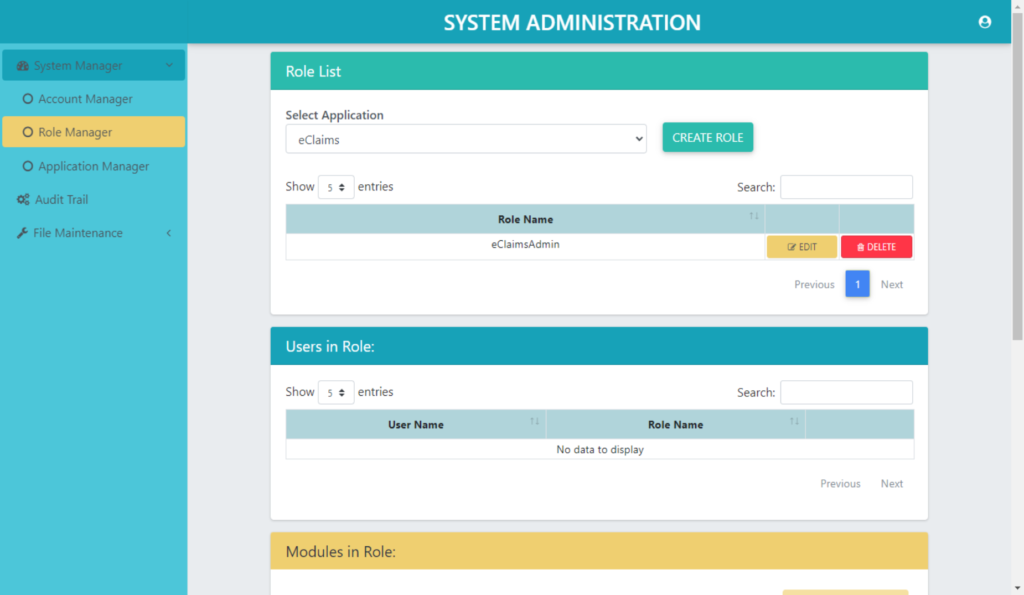
Systems Manager
System Manager provides a System level of security to protect against unauthorized access of the system. It manages the Role & Access Role – Based Access Control ( RBAC ) to provide access only to Authorized Users. Unauthorized user cannot access sensitive data of the system.
A User can be a member of one or more roles. The application can use role membership to determine whether a User is authorized to perform a requested action. System Manager has other security & management functions embedded in the modules such as Account Manager, Role Manager, Application Manager, Audit Trail and File Maintenance.